Some researchers think there is a link between vitamin D levels and coronary artery disease (CAD). CAD is the term for the type of cardiovascular disease with progressive closing of arteries that supply blood to the heart. It’s also known as atherosclerotic heart disease or atherosclerosis. If a critical artery closes completely, the result is a myocardial infarction, or heart attack.
Coronary artery disease is usually a silent disease. The first sign a person gets may be the sudden severe chest pain of a heart attack, or even sudden death.
Cholesterol and coronary artery disease
Coronary artery disease results from years of accumulating fat and cholesterol in the walls of the arteries, called an atheromatous plaque. This produces a narrowing of the artery at the site of the plaque that eventually closes off the artery, as shown in the following diagram.
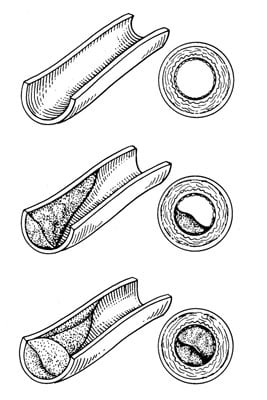
The atheromatous plaque develops in the following way:
Damage occurs in the inner lining of the artery (the epithelium) due to high blood pressure, diabetes, smoking, or increased cholesterol levels.
White blood cells called monocytes come to the damaged area, attach, and creep under the cells lining the artery. These cells then transform into macrophages (large cells) that produce signals that cause local inflammation called cytokines.
Macrophages accumulate fat, especially oxidized fat (similar to what happens when fat goes rancid). This accumulation of fat and cells is called a fatty streak.
The fatty deposits and white blood cells grow and send signals to other cells in the artery to divide and multiply. As a result, the lesion begins to stick out into the lumen, the opening of the artery that blood flows through.
Blood platelets can accumulate and form clots on the irregular surface of the plaque. The clot can remain there and clog the artery, or break off and lodge in a smaller artery, completely closing off blood flow beyond it. When this happens, the tissue supplied by that artery may die if the obstruction is not opened.
At very late stages of the disease, calcium is deposited in the walls of plaques, and cells in and around the plaque cause calcification. This can be seen in the artery by an X-ray. The calcification makes the artery brittle and hard to repair.
Vitamin D’s effect on coronary artery disease
There isn’t a definitive answer regarding the role of vitamin D in CAD; however, researchers think that vitamin D could be important in three ways:
Calcium deposits in arteries: The accumulation of calcium in arteries is a feature of the late stages of atheromatous plaque formation. Because vitamin D is so crucial for the control of calcium and bone metabolism, people have worried that a high vitamin D status might make the plaque calcify sooner or faster.
In fact, one symptom of vitamin D toxicity is that soft tissues can accumulate calcium and calcify like bone. In contrast, when 25-hydroxyvitamin D is high but not at toxic levels, some studies show it may even protect against calcium deposits in arteries.
Cholesterol reduction and vitamin D: Many doctors feel that controlling serum cholesterol and fat levels is critical to reducing the risk of cardiovascular diseases. The goal is to reduce the serum level of cholesterol, particularly a type called low-density lipoprotein cholesterol (LDL-C), and a type of fat called triglycerides. Other benefits can come from increasing a type called high-density lipoprotein cholesterol (HDL-C).
When a person has high cholesterol, cholesterol-lowering drugs called statins are given. These drugs block the production of cholesterol; however, there are some effects of these drugs that are not understood. Some have argued that they have beneficial effects on cardiovascular disease because of either a calcitriol-like (active vitamin D-like property or because they raise serum 25-hydroxyvitamin D levels).
There’s some new evidence that suggests vitamin D deficiency can decrease insulin sensitivity. This is part of a condition called the metabolic syndrome, an early stage of diabetes that increases a person’s chance of getting cardiovascular disease by raising LDL-C and triglyceride levels while lowering HDL-C levels. If it’s true, improving vitamin D status could reduce the risk of cardiovascular disease indirectly by improving insulin sensitivity.
Levels of vitamin D and inflammation: Vitamin D affects the immune system, resulting in changes that suppress how much inflammation the immune system causes while fighting an infection. Cardiovascular disease, particularly coronary artery disease, leads to localized inflammation. The macrophages in plaque produce cytokines that cause damage to healthy cells and make other cells in the artery multiply. This contributes to blocking the artery.
Because of this, several researchers have wondered if suppressing the production and negative effects of cytokines might be a mechanism used by vitamin D to prevent cardiovascular disease. A number of studies suggest that this might be true.

