The following discussion explains how diabetes affects your body. It’s good to know what’s happening before you dive into how to manage and treat diabetes.
Getting the lowdown on blood glucose
Diabetes is a disorder in which the amount of glucose, also called sugar, is too high in the blood. When you were diagnosed with type 2 diabetes, you were probably told that your blood glucose was sky high. But why would your blood glucose be high?It all comes down to eating — that amazing topic that everyone likes to obsess about. When you eat food, your body breaks that food down into glucose, and then the glucose travels in your bloodstream to waiting cells. That glucose really wants to get out of your blood and into your cells because that’s how you get energy. That’s the goal!
Insulin is a hormone that helps move glucose from your blood to inside your cells. However, people with type 2 diabetes don’t make enough insulin or aren’t as sensitive to that hormone. Therefore, the glucose gets trapped in the blood and can’t get inside your cells. Then high blood glucose — diabetes — happens.
Glucose is just a simple form of carbohydrate. The simplest carbohydrates are sugars, and the simplest sugar is glucose. It’s your body’s main source of energy, used to power everything from getting up in the morning to taking your dog for a walk. Is it blood glucose or blood sugar? Actually, they’re the same thing. Blood glucose is simple sugar. So, you may hear people say their “sugars” are too high or their blood glucose is too high. Blood glucose is the more technical term; sugar is the more colloquial term.
The mighty hormone insulin
You’ve probably heard of insulin, and you may associate it with injections or an insulin pump. We usually think of that as the synthetic or man-made medication. But the hormone in your body is also insulin. And it’s one of the most important hormones for helping you metabolize your food and get energy.Specialized beta cells in the pancreas make insulin. The pancreas, which is totally essential and underappreciated (until it stops working), is little, about 6 inches long, and sits right behind your stomach.
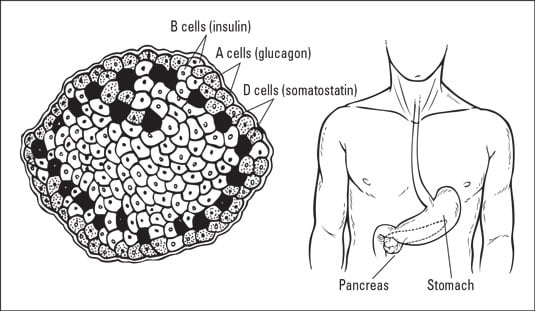 Illustration by Kathryn Born, MA
Illustration by Kathryn Born, MAThe pancreas and its specialized cells.
The pancreas has islet cells that include both beta cells, which make insulin, and alpha cells, which make another hormone called glucagon. Both insulin and glucagon are important for metabolizing food.
Beta cells are the only cells that make insulin. In type 2 diabetes, several things are happening with those beta cells:
- The beta cells don’t work well. They don’t make as much insulin as they’re supposed to.
- There may be fewer beta cells than usual.
- The beta cells that are making all the insulin get burned out (super tired) and eventually make less insulin. It’s a cycle in which insulin production can get worse over time.
It’s a double whammy: Your pancreas makes less insulin, and yet you need more insulin than ever before. It’s not a good combination.
If your body doesn’t make enough insulin or if you have insulin resistance, your glucose can’t get inside your cells and builds up in your blood. This is called high blood glucose. It’s the key factor that defines diabetes.
Scientists are still trying to figure out why beta cells fail or die — and also why the body becomes less sensitive to insulin. If they can get to the bottom of those questions, we’re on our way toward a cure for type 2 diabetes.
In the meantime, scientists know that insulin sensitivity can be improved by exercise. Just a short bout of exercise can improve insulin sensitivity for up to 24 hours. It’s another amazing effect of breaking a sweat besides burning calories.
Insulin is a hormone that helps your cells use glucose for energy. It’s made by beta cells in the pancreas. People with type 2 diabetes may not make enough insulin or may not be as sensitive to insulin — or both.

