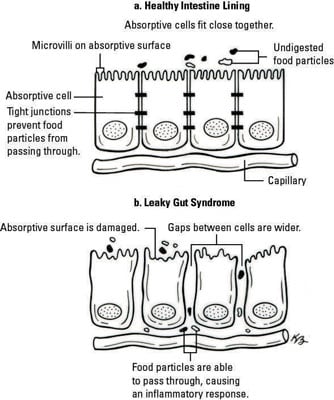
Intestinal dysbiosis is a general term that refers to an unhealthy small intestine due to an imbalance in gastrointestinal bacteria. This can cause adrenal fatigue. You see the loss of the integrity of the intestinal cells; the tight junctions are worn down, and gaps exist between the cells. The cells have lost the glue that keeps them working well.
Among the factors that can cause intestinal dysbiosis are antibiotic and other medication use and the overgrowth of a yeast called Candida.
How antibiotics can throw off the intestinal ecosystem
Antibiotics can really disrupt the delicate balance of the intestinal ecosystem, killing off the good bacteria that keep the bad bacteria at bay. Even one dose of an antibiotic can have a significant effect on the ecosystem of the intestine.
Unfortunately, healthcare practitioners prescribe huge amounts of antibiotics. Most people expect that they'll get an antibiotic when they see their doctors, and some parents practically demand that their children receive antibiotics regardless of whether they're warranted. The medical profession is just starting to realize the negative effects of the overuse of antibiotics.
Be aware of some of the clinical consequences of antibiotic use:
Diarrhea: Antibiotics can cause diarrhea, a condition called antibiotic associated colitis. Luckily, this can resolve when you stop using the antibiotic.
Clostridium difficile colitis: See the nearby sidebar for details on this inflammatory condition.
Yeast overgrowth: Candida overgrowth can lead to weakness and fatigue, flu-like symptoms, fungal skin rashes, weight gain, and abdominal bloating.
Which antibiotics do you need to be aware of? Well, any class of antibiotics has the propensity to alter the intestinal flora, but certain classes — including the penicillins, cephalosporins, fluoroquinolones, and clindamycin — have been recognized as causes of antibiotic associated colitis and Clostridium difficile colitis.
Think of your immune system as a part of you that matures and develops as you do. You can avoid damaging it by minimizing antibiotic use. Of course, we're not saying that a patient shouldn't be prescribed an antibiotic when absolutely needed, but be cautious, especially with children.
The next time an antibiotic is a treatment option, both you and your practitioner need to ask, “Is this antibiotic really necessary? Would a natural remedy work to boost the immune system and help fight off that infection?”
If an antibiotic is truly the best treatment, ask whether you can take probiotics (beneficial microorganisms) with it to help replenish the good bacteria. This helps minimize the degree of damage that the antibiotic does to the intestinal tract.
How Candida fungus can lead to intestinal dysbiosis
Bacteria aren't the only organisms in the intestinal ecosystem. Candida, the most common genus of yeast (a fungus), is also in your small intestine. It's usually present in very small amounts, and the beneficial bacterial flora help keep the level of Candida in check.
Overgrowth of Candida in the intestine is a problem largely unrecognized in the United States. The factors contributing to the overgrowth of Candida are
The overuse of antibiotics
A Western diet, an acidic diet, and or a diet high in sugar
Stress
Chronic illness and malnutrition
Diabetes mellitus (a significant risk factor)
The symptoms of Candida overgrowth (and how to reverse them) can include the following:
Weakness/fatigue: One of the main symptoms of Candida overgrowth is weakness and fatigue that simply doesn't get better and persists for a long time. The key to treating this is recognizing the symptom early on in conjunction with other symptoms.
Flu-like symptoms, including arthralgias (joint pains) and myalgias (muscle pains) that can persist and even worsen over time: Many things can cause leaking of tight cell-to-cell junctions, and Candida is one of them. Candida can secrete fungal toxins called mycotoxins that can leak out into the bloodstream and have systemic effects, including joint pain and flu-like symptoms.
The common recommendation from modern practitioners? Avoid foods that are high in sugar.
Fungal skin rashes: The presence of skin rashes that don't go away, along with recurrent yeast infections, can be connected with Candida overgrowth syndrome.
How do you know if you have a fungal skin rash? Well, general characteristics of fungal skin infections are skin lesions that are scaly, red, and really itchy. Usually they're present on a certain area of the body, as in athlete's foot. They can also occur on the chest, the arms, or the legs.
The short-term treatment of this condition includes topical antifungal medications such as clotrimazole (Lotrimin). Your healthcare practitioner may also prescribe a medication that treats fungal infections, a common example being fluconazole (Diflucan). The long-term treatment is the use of natural antifungal agents, including garlic and olive leaf, as well as eliminating sugar from your diet.
Weight gain: Maybe you've decreased your caloric intake and are exercising more (congratulations!), but you're still having a hard time losing weight. Maybe you're even gaining weight. If so, suspect Candida overgrowth. Simply put, if you don't eliminate the yeast overgrowth in the intestine, losing weight will be difficult, if not impossible. One of the keys to combating fungal overgrowth is restricting sugar intake.
Abdominal bloating: Fungal overgrowth in the intestine can cause bloating and distention. Yeast rises, especially when your diet contains excess sugar. That's why you can end up with an abdomen that looks like a giant loaf of bread.

